marzNC
Angel Diva
Post #4 includes a video about the first patient to undergo BEAR. The young man tore his ACL while skiing during the 2015-16 season.
The repair surgery includes adding a special blood-soaked sponge as a "scaffold" to help the ligament heal naturally. Normally the synovial fluid inside the knee prevents blood from staying around during the healing process. The ACL is the only ligament completely inside the knee. This repair process works best on younger patients based on research in animal models. Younger patients are at higher risk for failure when ACL reconstruction surgery is performed. The Phase 2 trial recruited patients ages 18-35.
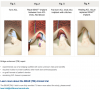
The repair surgery includes adding a special blood-soaked sponge as a "scaffold" to help the ligament heal naturally. Normally the synovial fluid inside the knee prevents blood from staying around during the healing process. The ACL is the only ligament completely inside the knee. This repair process works best on younger patients based on research in animal models. Younger patients are at higher risk for failure when ACL reconstruction surgery is performed. The Phase 2 trial recruited patients ages 18-35.



